Primary Care First Model
Primary Care First is a voluntary alternative five-year payment model that rewards value and quality by offering an innovative payment structure to support the delivery of advanced primary care. In response to input from primary care clinician stakeholders, Primary Care First is based on the principles underlying the existing Comprehensive Primary Care Plus (CPC+) model design: prioritizing the clinician-patient relationship; enhancing care for patients with complex chronic needs and focusing financial incentives on improved health outcomes.

Model Goals
Primary Care First aims to improve quality, improve patient experience of care, and reduce expenditures. CMS believes that the model will achieve these aims by increasing patient access to advanced primary care services. PCF has elements specifically designed to support practices caring for patients with complex chronic needs or serious illness. The specific approaches to care delivery are determined by practice priorities. Practices are incentivized to deliver patient-centered care that reduces acute hospital utilization or total per capita cost. PCF is oriented around five comprehensive primary care functions:
- Access and continuity
- Care management
- Comprehensiveness and coordination
- Patient and caregiver engagement
- Planned care and population health
Primary Care First aims to be transparent, simple, and hold practitioners accountable by:
- Providing model payments to practices through a simple payment structure, including:
- A flat payment that encourages patient-centered care, and compensates practices for in-person treatment;
- A population-based payment to provide more flexibility in the provision of patient care along with a flat primary care visit fee; and
- A performance-based adjustment providing an upside of up to 50% of model payments as well as a small downside (negative 10% of model payments) incentive to reduce costs and improve quality, assessed and paid to practices on a quarterly basis.
- Providing practice participants with performance transparency, through identifiable information on their own and other practice participants’ performance to enable and motivate continuous improvement.
Learn more: https://innovation.cms.gov/innovation-models/primary-care-first-model-options.
SHARE Daily Reports on all Medicare Beneficiaries
Want to be notified in the last 24 hours of when your Medicare patients have been Admitted/Discharged from the emergency department (ED) and Inpatient discharged?
** Please note SHARE will need your clinics Medicare attribution list with specific data elements to begin the daily 24-hour report.
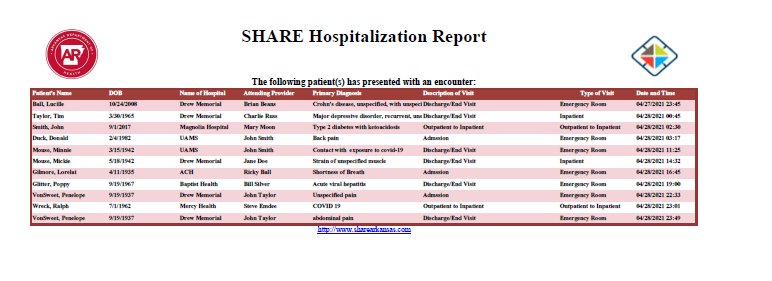
SHARE Hospitalization Report Example